Hospitals consume significantly more energy than other buildings and facilities of similar size and therefore hospital energy savings can be tremendous. The average 200,000 ft2 facility spends about $13,600 per bed, or roughly $680,000 annually, on energy costs. Why so much? Operating twenty-four hours a day, thousands of employees, patients, and visitors cycle through campus buildings daily. Additionally, hospitals maintain high ventilation rates to lessen the risk of microbial contamination; the conditioning requirements of this outdoor air represents significant energy usage. Further, the use of sophisticated imaging equipment, electronic health record systems and other operations generates heat that must be compensated for via the site’s cooling load. Lastly, many hospitals are built over time, creating a mixture of fixtures, equipment, management systems which can be a burden on utility bills if not controlled with energy efficiency in mind.
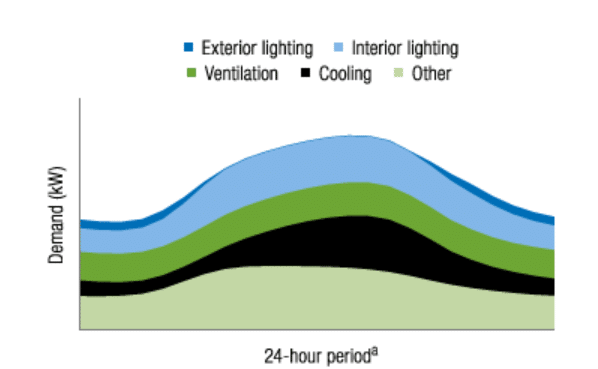
It is no surprise then that hospital operations teams are continually seeking to improve energy efficiency and reduce operating costs. Hourly hospital energy consumption data from the Orlando Utilities Commission underscores that cooling, ventilation and lighting represent the largest opportunities for reducing electricity costs in healthcare facilities. Let’s take a look at how to reduce spending in those areas.
Ventilation & Hospital Energy Savings
The large quantity of outside air necessary for proper ventilation requires an increased amount of energy to condition. While ventilation can limit the spread of airborne pathogens throughout a healthcare facility, these higher ventilation rates come at an increased energy cost.
Many hospitals ventilate spaces as if they were occupied at full capacity. For non-critical spaces that have fluctuating capacity like indoor parking garages, lobbies, and cafeterias, energy savings can be realized by reducing ventilation when these spaces are not full. A demand-controlled ventilation (DCV) system senses the amount of carbon dioxide in the space’s return airstream and uses it as an indication of occupancy. It then adjusts how much outside air is brought into the space based on the current occupancy level. By modulating this process, DCV reduces the amount of outside air that must be heated or cooled and the amount the fans must run to move that air.
DCV systems rely on occupancy to reduce the operating speed of the supply and exhaust fans when rooms are unoccupied. When there are issues with this equipment that go undetected, however, energy is used in excess. Periodical recommissioning can ensure that dampers, actuators, or control cycles aren’t getting stuck open or failing to operate correctly.
Lighting & Hospital Energy Savings
The lighting demands of hospitals are complex due to their round the-clock nature. Both low-tech and high-tech solutions, however, exist for lighting controls that can greatly reduce energy costs.
One simple, low-tech reduction solution is lighting awareness campaigns that train staff to turn off lights when rooms are not in use. De-lamping is an additional, lower-cost way to reduce energy. As the name suggests, it’s done by removing unnecessary light bulbs and fixtures in areas that are producing greater-than-needed illumination. De-lamping in areas of excessive illumination immediately reduces energy consumption while also decreasing cooling load needs in warmer months. Further, replacing traditional bulbs with LEDs can save upwards of 50% percent of the energy costs of using traditional light bulb.
High-performance lighting systems can significantly reduce energy usage by ensuring electric lighting is used only when necessary. Installing occupancy controls, dimmers, and daylighting controls in offices, break rooms, storage rooms, and restrooms can have a dramatic affect in reducing lighting electrical use.
Space cooling & Hospital Energy Savings
While ventilation and lighting improvements can reduce energy costs, chiller plants are the single largest consumer of energy in most health care facilities. Hospital cooling, therefore, bears the brunt of utility usage and optimizing the chiller plant is one of the greatest means of short and long-term reduction of energy use.
Optimizing the cooling system ensures that hospital conditioning requirements are being met at the lowest possible cost (or kW/ton). A system, however, must be designed for optimization-new equipment or analytics packages will have an energy impact but fall short of realizing optimization savings.
To assess a hospital’s candidacy for optimization savings, an audit should be performed to assess how the cooling system and equipment is being used, how the hospital’s various systems and machines either do or do not work together, how current operation strategies are impacting energy performance, and what pragmatic solutions could be implemented that will both reduce consumption and pay back quickly.
Xpress® & Hospital Energy Savings
One such solution is tekWorx Xpress®, a combination of adaptive control algorithms and Tridium Niagara N4 hardware that optimize a hospital’s chilled water plant equipment (air-handling units, fan coils, chillers, cooling towers, etc.) in real-time. These optimization algorithms continuously adjust equipment sequences and key setpoints based on such parameters as occupancy level and outdoor temperature to continually maximize the system efficiency while maintaining space cooling conditions throughout the hospital, including operating rooms. An integrated dashboard allows facilities staff to monitor the overall efficiency of the chilled water system from anywhere at any time.



